Author: Lilian Kaivilu | Producer: Dorothy Okemo
In our blog series “Four tales from Narok County, Kenya” we put the spotlight on the healthcare situation of people living in Narok with a special focus on sexual and reproductive health (SRH).
Where there’s little to no money for health, a hard-working nurse struggles to serve the 5,000 people in his sub-county and a volunteer with a background in tourism steps in to educate communities on SRH. Without financial support, youth centres have to close, leaving adolescents with sexually transmitted diseases to seek help at neighbouring counties’ facilities in order to prevent stigma from their own communities. Facing a lack of education on sexuality and contraceptives, many young girls experience unprepared motherhood and are forced to abandon their education all together. But among all these challenges there are people who fight for better knowledge of SRH Rights and improved access to medicines.

Growing up, Robert Magero watched his mother serve at a local health facility. He keenly followed her encounters as she cleaned the hospital wards and corridors. “I saw the challenges my mother witnessed in the hospital. This inspired me to want to become a doctor as I believed I would address the challenges at that position,” says Magero.
As his Form Four grades did not qualify him to pursue a direct course in medicine, a determined Magero opted for a Diploma in Clinical Medicine at St Luke’s Nursing School, a Catholic sponsored medical training college. After 13 years of work, he became the clinical officer and only staff member at the Etereti Dispensary in 2019.

According to the Kenya National Population Census 2019, Ololung’a has a total population of 5,609. Magero’s dispensary is the only one available to them. Tuesdays and Thursdays are the local market days in Olulung’a area. This means that the locals do not make hospital visits on such days. But for the rest of the week, Magero sees about 50 patients per day.
As he lives in Narok town, he has a daily commute of more than an hour. Still, to community members, a nurse is expected to serve them at any time of need. “Community members may not understand; regardless of the time of night,” his sense of frustration is evident when he tries to explain the feeling that comes with abusive words from patients who often present with less serious complications that could have waited. To the community, this is a doctor and anytime is treatment time.

In the time of COVID-19, there is need for more caution, including proper hand washing and keeping physical distance. But as the only health worker here, Magero has no control over who walks in and whether they’ve washed their hands or not. “Sometimes a patient comes straight into the consultation room without even washing their hands. I can’t chase them away. I also cannot be outside monitoring who has or hasn’t washed their hands,” he says. To stay safe, Magero regularly uses hand sanitiser.

Despite the fast-spreading COVID-19 pandemic, locals here have not fully adapted to the government regulations of hand washing and wearing face masks. According to Magero, the nearest place for the locals to buy masks is 20 kilometers away. It costs Sh300 one way to access the shopping centre, while a mask costs Sh100. This is a lot of money, considering that the lowest paid government worker earns about 449Kshs per day in wages, and puts most locals off buying masks.

On the day we visited his health facility, blood stains are evident under the only bed in the dispensary. Magero, the only nurse in the hospital, had a patient with a still birth the night before. “It was a tough choice for me. The patient came at a very late stage and unfortunately had a still birth. Referring her to the nearest facility wasn’t an option as she would have had more challenges on the way,” says a visibly distraught Magero.
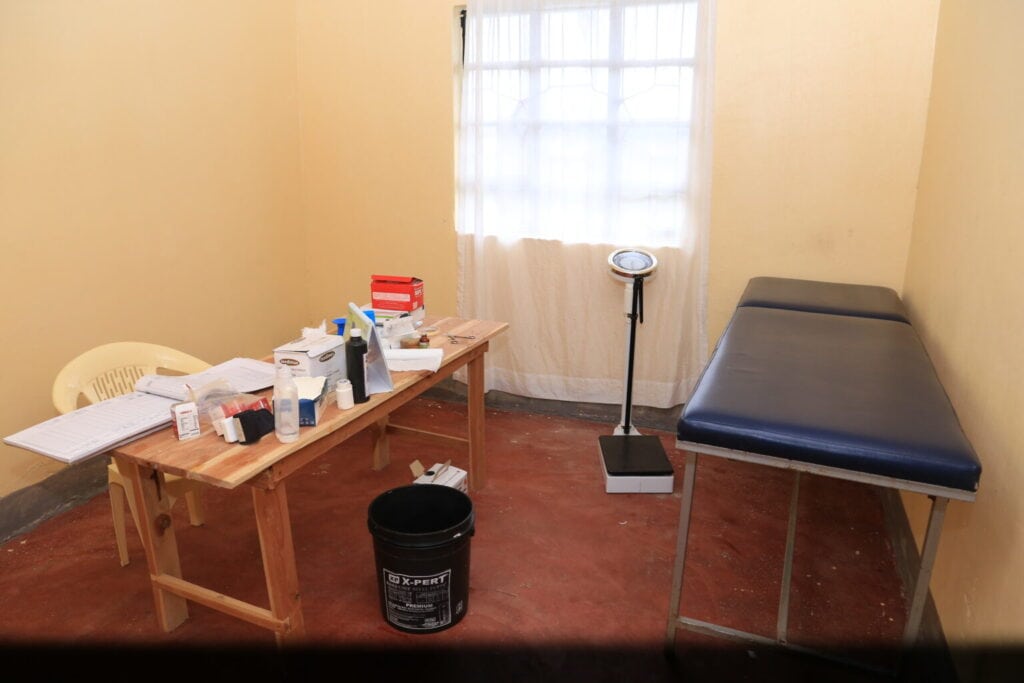

On the subject of pregnancies, Magero condemns the lack of adequate essential drugs, such as folic acid, and proper infrastructure, especially when mothers have to be referred to a higher-level facility. “The same bed that I use to palpate a pregnant mother is the same one that I use to administer a drip. It is discouraging sometimes to refer a patient for a case that you could have done just because of lack of the necessary commodities,” he laments.

Although the dispensary is otherwise relatively well structured with a store, consultation room and a treatment room, medical supplies are a challenge here, too. Essential medicines, such as supplements and immunisation drugs are unavailable, especially towards the end of the financial year. This past financial year, he says, the facility received only $600 per month to cater for the day-to-day operations. Water supply is not assured, as the hospital depends on rainwater. With only one water tank in the compound, Magero is forced to buy the resource from water vendors. A 20-litre jerrycan costs between Sh20 and Sh30. This is a lot, considering Magero’s budget of $600 a month to manage the facility. Each day, he buys at least five jerrycans and pays a total of $10, pushing up his expenses for water to $300 per month—half of his budget.

According to Sexual and Reproductive Health Commodities: Availability, Affordability and Stockouts, a 2019 report by Health Action International (HAI) and Medicines Transparency Alliance (MeTA) Kenya under the lead of Dorothy Okemo, availability of SRH in in the country was 43% in 2019, an improvement from the previous year. The report further reveals that availability of SRH commodities was higher in the public (48%) and mission sectors (46%), while the private sector had a lower availability (36%).

But for Etereti dispensary, a public facility, long procurement procedures have seen the facility receive drugs twice a year or less. The dispensary had last received drug supplies in July 2020—the previous delivery was in July 2019. Magero dreads running out of essential commodities—as the only nurse he already struggles to serve everyone in his community, but without drugs he can only do so much.
At the end of 2015, Health Action International (HAI) teamed up with Amref Health Africa, the African Centre for Global Health and Social Transformation (ACHEST), Wemos and the Dutch Ministry for Foreign Trade and Development Cooperation to form the Health Systems Advocacy (HSA) Partnership, which ran until the end of 2020.
Throughout this five-year programme, the HSA Partners contributed to stronger health systems that enabled people in Sub-Saharan Africa to equitably access high-quality Sexual and Reproductive Health (SRH) commodities and services. As part of our work on SRH, we contributed to capacity building by equipping civil society actors and health stewards with needed knowledge, technical skills and tools to develop and implement evidence-based advocacy strategies.
Our work in this field drew upon our research and advocacy expertise. In collaboration with our in-country partners, HEPS Uganda, Medicines Transparency Alliance (MeTA) Zambia and MeTA Kenya, we studied the price, availability, and affordability of SRHC in facilities across Kenya, Uganda, Zambia and Tanzania. These findings formed the basis of our advocacy work with our in-country partners. Our blog series “Four Tales from Narok County” shows that there is more work to be done with our in-country partners. Therefore, Health Action International is looking for new funding opportunities to pursue the collaboration with multi-stakeholder platforms and grassroot organisations in their fight for SRH rights.